How Do IUDs Work And Are They Safe?
An intrauterine device (IUD) is a type of birth control a healthcare provider inserts into your uterus. IUDs are the most commonly used type of long-acting reversible contraception (LARC). Once an IUD is inserted, you don’t have to worry about birth control until it’s time to replace it (three to 10 years, depending on the brand). LARCs, which include IUDs and contraceptive implants, are the most effective form of birth control that doesn’t require surgery. If you do decide to become pregnant, your provider can remove your IUD.
Unlike other forms of contraception, like condoms, IUDs don’t prevent sexually transmitted infections (STIs). You can use an IUD with condoms to prevent pregnancy while also reducing your risk of contracting an STI.
What are the different types of IUDs?
There are two kinds of IUDs, copper IUDs and hormonal (levonorgestrel) IUDs. Both have plastic frames that open into the shape of a T once inside your uterus. They have strings attached at the bottom that extend into your vagina so that your provider can remove your IUD as needed. The FDA has approved five brands of IUDs: Paragard® (copper) and Mirena®, Liletta®, Kyleena® and Skyla® (hormonal).
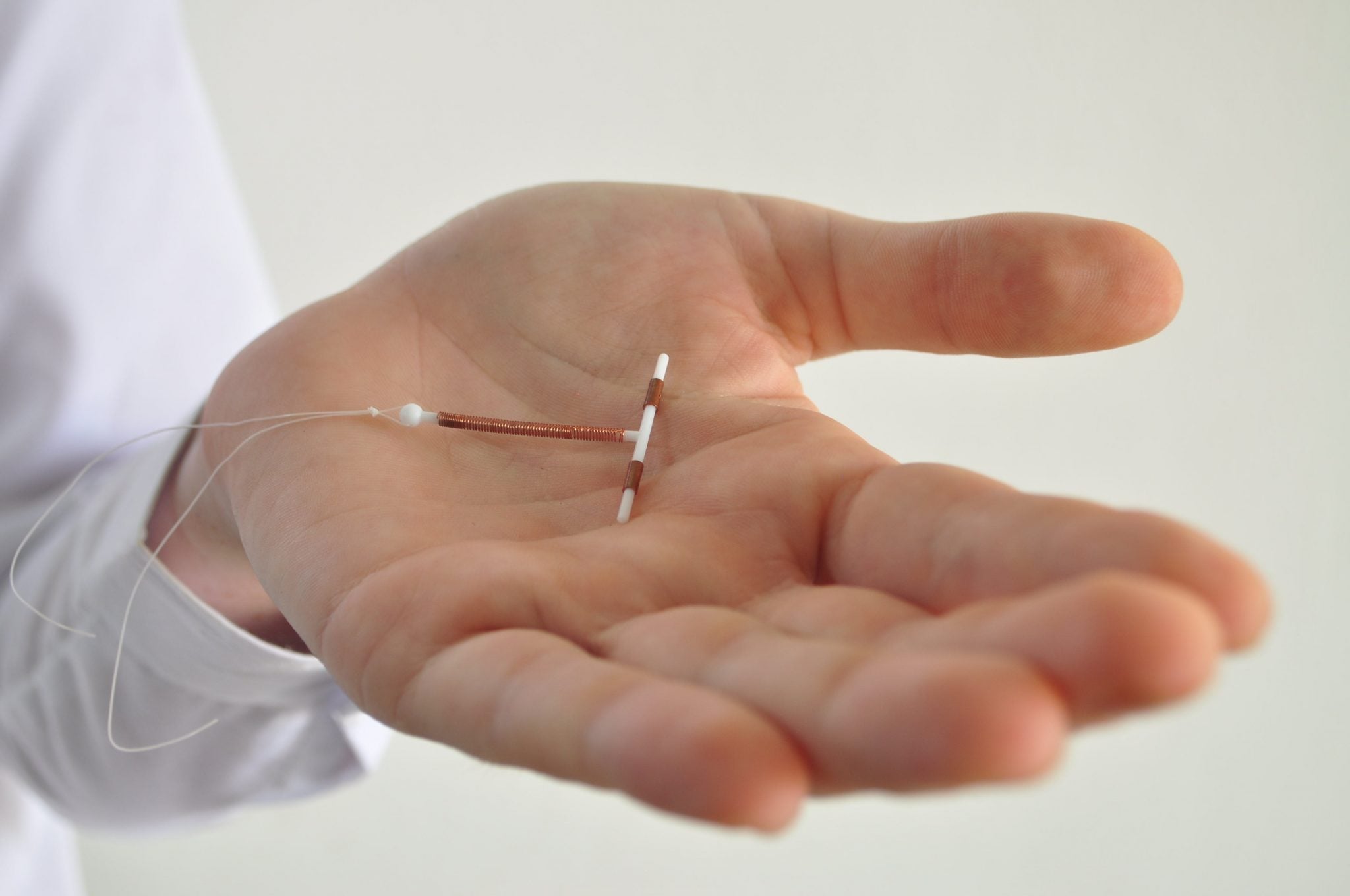
Copper IUDs: Paragard’s IUD has a thin copper wire that coils around the stem part of the “T.” The stem ends in a smooth ball that prevents your cervix from getting punctured when your provider inserts your IUD.
Hormonal (levonorgestrel) IUDs: The top part of the “T” contains the progestin hormone levonorgestrel, which flows through the stem. Progestins are a synthetic version of progesterone, a hormone that occurs naturally in your body. Mirena and Liletta are slightly bigger around than Kyleena and Skyla.
Both types contain elements that cause them to show up during imaging procedures. Your provider can check your IUD during wellness visits to ensure it’s positioned correctly.
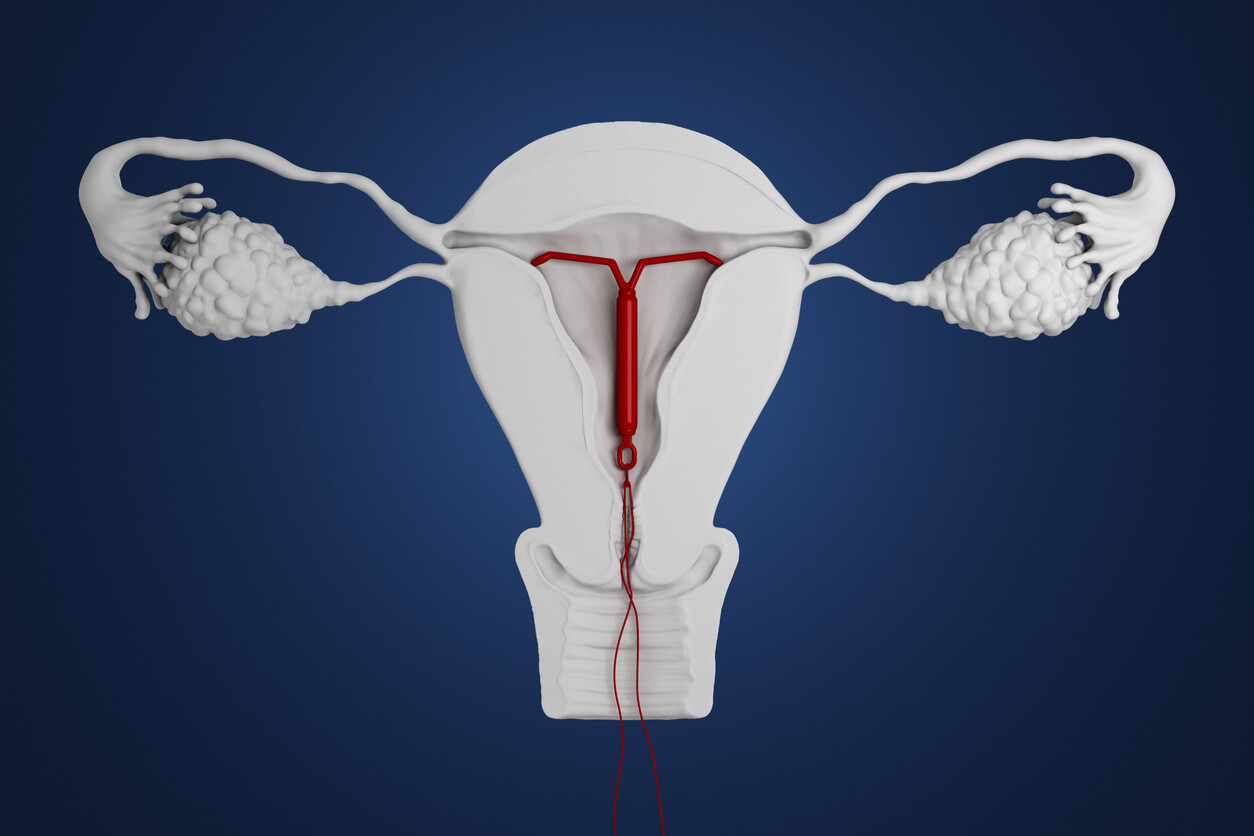
How do IUDs work?
All IUDs trigger an immune response. Your body recognizes an IUD as an invader and springs into action to defend itself. This process results in inflammation. Inflammation in your uterus creates an environment that’s toxic to sperm. As a result, sperm can’t reach your fallopian tubes to fertilize an egg. The specific properties of copper and hormonal IUDs also prevent sperm from leaving your uterus.
Copper IUDs: Heighten the inflammatory response, causing your uterine lining (endometrium) to become inflamed. Even if sperm were to fertilize an egg, your uterine lining would make it difficult for a fertilized egg (embryo) to implant there and develop.
Hormonal IUDs: Release small amounts of the progestin hormone levonorgestrel over time. Levonorgestrel thickens your cervical mucus, making it harder for sperm to swim to your fallopian tubes. It also thins your uterus lining and partially suppresses your ability to release an egg during your menstrual cycle.
Not all hormonal IUDs contain the same amount of levonorgestrel or have the same release rate. For example, Mirena and Liletta release more progestin than Kyleena and Skyla. Talk with your provider about which brands work best for you.
What happens during the insertion?
Inserting an IUD takes fifteen minutes or less. Your provider can perform the procedure during an office visit. You’ll be positioned on a table as if you were having a Pap smear, with your knees bent, legs opened and supported in stirrups. You may be given a numbing injection near your cervix to lessen any pain or discomfort. Your provider will use a speculum to widen your vagina. You may feel mild to intense cramping when your provider inserts the IUD.
How soon will my IUD start working?
Paragard starts working immediately. Hormonal IUDs begin preventing pregnancy depending on where you are in your cycle. If you’re on your period, they start working right away. If you’re not on your period, it may take a week for them to offer you protection. Use other forms of birth control as you wait for your IUD to take effect.
What are the risks of using an IUD?
IUDs are considered both safe and effective. Complications — while rare — may include:
Expulsion: Your IUD may slip out of your uterus. When this happens, it usually occurs during your period, within the first few months after it’s been inserted.
Perforation: The uterine wall can be pierced during insertion.
High-risk pregnancy: Your chances of becoming pregnant are slim. On the off chance that you do become pregnant, your pregnancy will be considered more likely to result in pregnancy complications. Making sure that you don’t use your IUD beyond its expiration date can prevent pregnancy.
Infection: Bacteria can enter your body when your IUD is inserted, causing an infection. Infections are most likely to occur within the first 20 days of insertion. Your healthcare provider will clean your cervix during IUD insertion to lower the risk.
In Conclusion
Intrauterine devices (IUDs) are a safe, effective and convenient form of birth control. Once inserted, they can prevent pregnancy for several years. Weigh the pros and cons of getting an IUD with your healthcare provider. They can help you decide if an IUD is the best option for you. They can also recommend the type of IUD that’s best for you. If you do decide to use an IUD, don’t forget to use another method to prevent STIs.



